Are you or a loved one experiencing…?
🌀Confusion & mental fog 😔Personality changes
💤Day-night sleep reversal 🗣️Slurred speech
🤝Hand tremors 🔑Forgetfulness
These could be signs your liver is affecting your brain
When the Liver
Suffers,
the Brain Speaks.
Are We Listening?
Liver disease can silently affect your brain — causing confusion, memory issues, and mood changes. This condition is called Minimal Hepatic Encephalopathy (mHE), and the good news is: it's detectable and treatable.
Learn About mHE
We're here for you
This Site Is For You — Wherever You Are In This Journey
love, or providing professional care — we have the information you need
in plain language.
For Patients
You have cirrhosis or liver disease and want to understand what's happening to your brain — and what you can do about it.
- Understand what mHE is
- Recognize early warning signs
- Learn about your treatment options
- Know when to call your doctor
- Take the free risk quiz
For Family Members
Your loved one has liver disease and you're noticing subtle changes in their behavior, memory, or mood - but don't know if it's serious.
- Signs to watch out for
- How to talk to your loved one
- When to contact their doctor
- How to support daily routines
- Safety tips at home
For Caregivers
You're a healthcare professional or home caregiver supporting someone with liver disease who needs clear clinical guidance.
- Screening tools for mHE
- Treatment protocols overview
- Daily care best practices
- Nutrition and hydration guidance
- When to escalate care
T H E C O N N E C T I O N
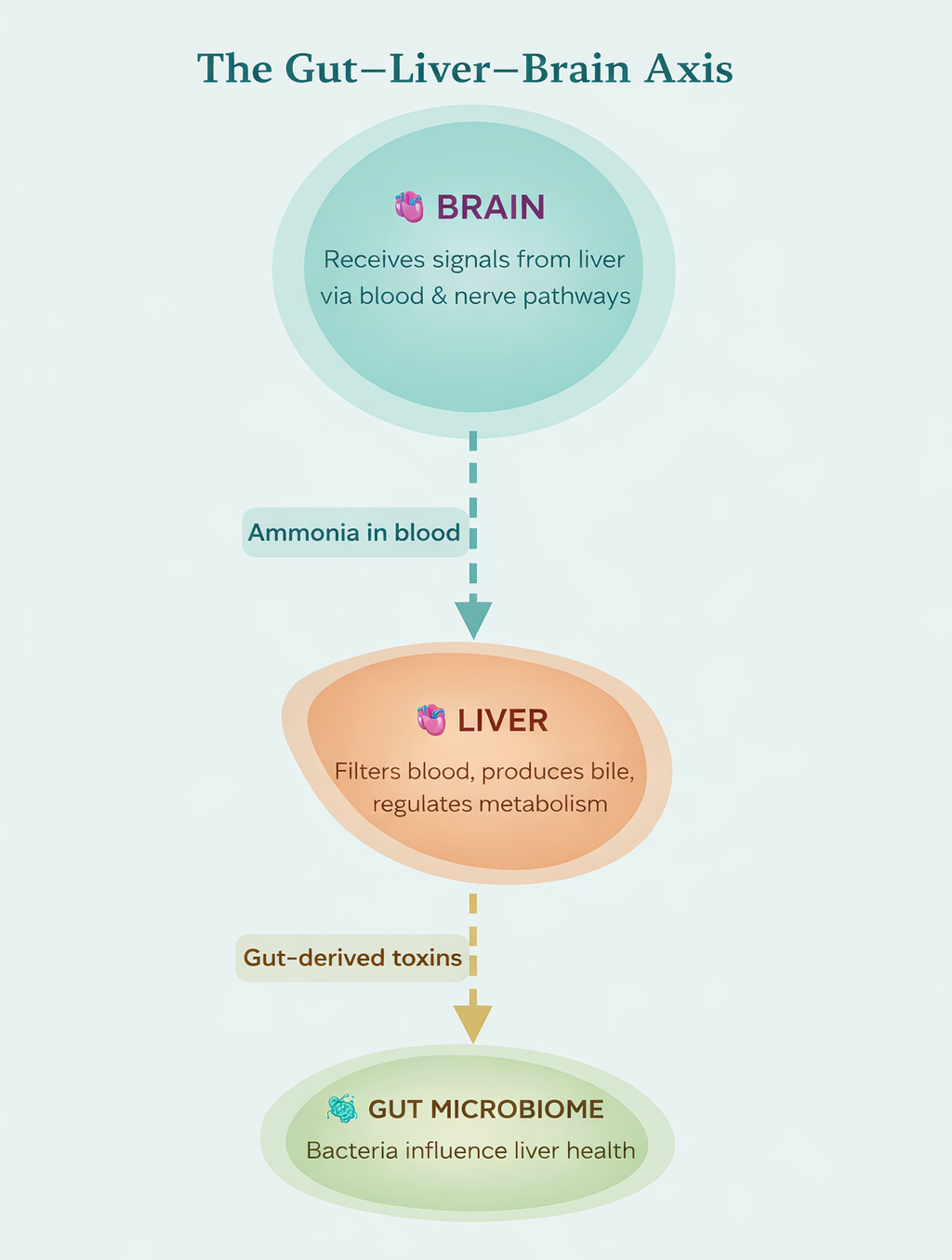
How Does the Liver Affect the Brain?
Think of your liver as the body's water treatment plant. When it's not working well, toxins build up and travel to the brain.
The Liver Filters Toxins
Normally, your liver cleans ammonia and other harmful substances from your blood before they can reach your brain.
Liver Disease Disrupts This
In liver conditions like cirrhosis, this filtering process breaks down. Toxins — especially ammonia — start to accumulate in the bloodstream.
Toxins Reach the Brain
These toxins cross the blood-brain barrier and begin disrupting how your brain cells communicate, causing the mental and behavioral symptoms of Hepatic Encephalopathy.
mHE Is the Earliest Stage
In minimal Hepatic Encephalopathy (mHE), the effects are subtle and easy to dismiss — but catching it early makes a significant difference.
Understanding the Condition
Two Types of Hepatic Encephalopathy
Hepatic Encephalopathy (HE) ranges from invisible early symptoms to
obvious signs. Catching it early — in the "covert" stage — gives the best
chance for recovery.
🤫 Covert HE (mHE)
This is the hidden, early stage. Symptoms are subtle and easily mistaken for stress, aging, or fatigue. The person looks and acts mostly normal, but is experiencing real changes in brain function that affect their quality of life and safety — especially driving.
🚨 Overt HE
This is the obvious, more advanced stage. Symptoms become hard to ignore: significant confusion, disorientation, slurred speech, uncontrolled shaking, extreme drowsiness, or even coma. This stage requires immediate medical attention.
Early Warning Signs
Whispers of mHE — Easy to Dismiss, Important to Catch
These subtle signs are often brushed aside as "just getting older" or "stress." But in someone with liver disease, they deserve attention.
🔑
Forgetfulness
Trouble remembering recent events, names, appointments, or where common items were placed.
🌫️
Mental Fog & Mild Confusion
Difficulty following complex conversations or instructions; feeling mentally slow or "not quite right."
🎯
Poor Concentration
Finding it hard to stay focused on tasks; becoming easily distracted; losing track mid-task.
🌙
Sleep Disruption
Day-night reversal — sleeping during the day and awake at night; or excessive daytime drowsiness.
Text
🚗
Slower Reactions
Subtle clumsiness or slower reaction times — particularly important for driving safety.
😠
Personality Shifts
Increased irritability, mild anxiety, or pulling away from social situations — uncharacteristic behavior.
Recognize any of these in yourself or a loved one with liver disease?
The Good News: mHE Is Treatable
dramatically better quality of life.
STEP 1
Detectable
mHE can be diagnosed with simple tests like the Critical Flicker Frequency (CFF) test. Routine screening in all cirrhosis patients is recommended and can reveal the condition even when there are no obvious symptoms.
STEP 2
Reversible
Treatment options include lactulose (a laxative that reduces ammonia absorption), rifaximin (an antibiotic), and dietary adjustments. Many patients see significant improvement in brain function with proper treatment.
STEP 3
Manageable
Long-term management through lifestyle changes — regular sleep, good hydration, avoiding alcohol, a protein-appropriate diet, and regular check-ins with your liver specialist — can protect your brain health.
"The sooner we act, the sooner the brain heals."
Are You At Risk?
FOR CAREGIVERS & FAMILY
How to Support Someone
With mHE
Caring for someone with liver-related brain symptoms can be
1️⃣ Know the Warning Sign
Learn to recognize when symptoms are worsening. Significant confusion, unresponsiveness, or unable to wake up requires emergency care immediately.
2️⃣Medication Management
Help ensure medications like lactulose are taken as prescribed. Track bowel movements — the goal is 2–3 soft stools per day with lactulose therapy.
3️⃣Safe Driving Conversations
Increased irritability, mild anxiety, or pulling away from social situations — uncharacteristic behavior.
4️⃣Dietary Support
Encourage adequate protein intake (don't restrict it unless told by a doctor), small frequent meals, and staying well hydrated. Avoid alcohol completely.
5️⃣Routine and Sleep
A consistent daily routine helps manage sleep inversion. Encourage daytime activity and avoid long naps to help restore normal sleep cycles.
5️⃣Take Care of Yourself Too
Caregiver burnout is real. Join a support group, ask for help from family, and speak to a counselor if you're feeling overwhelmed or isolated.
C O M M O N Q U E S T I O N S
Frequently Asked Questions
Plain-language answers to the questions we hear most often from patients
and families.
Yes — this is exactly the point. mHE is called the "invisible threat" because it presents with no obvious symptoms. However, it can still significantly affect quality of life, work performance, driving safety, and daily activities. Up to 50–80% of people with cirrhosis may have mHE. Routine screening is strongly recommended.
No. HE is not a psychiatric condition. It is a medical condition caused by toxins — particularly ammonia — building up in the blood due to liver disease and affecting brain function. It can cause mental and behavioral changes, but treating the underlying liver condition and clearing the toxins can reverse these changes.
mHE (Grade 0) is the subtle, early stage where symptoms are not obvious to others but detectable with specialized tests. Overt HE (Grades 2–4) involves clearly visible symptoms like significant confusion, disorientation, tremors, slurred speech, or even coma. Overt HE requires immediate medical attention.
mHE can often be significantly improved and in many cases reversed with appropriate treatment. Medications like lactulose and rifaximin reduce ammonia levels, while dietary and lifestyle changes support long-term brain health. The key is early detection — the earlier mHE is caught, the better the outcome.
This is an important safety concern. mHE can impair reaction time, concentration, and judgment — all critical for driving. Studies have shown increased accident rates in people with mHE. It's strongly advisable to discuss driving safety with the treating doctor, and in many cases, driving should be restricted until the condition is treated and reassessed.
mHE is diagnosed through neuropsychological tests. The Critical Flicker Frequency (CFF) test, Psychometric Hepatic Encephalopathy Score (PHES), and other computerized tests can detect subtle cognitive impairments that aren't obvious in a standard examination. Ask your gastroenterologist or hepatologist about getting screened.
Ways to Reach Us
Talk to Someone
You Don't Have to Figure This Out Alone
Our team connects patients, families, and caregivers with specialists who understand the liver-brain connection. Get personalized guidance — not generic answers.
📋 Most popular
Online Consultation Form
🗒️ Free & Anonymous
Take the Risk Assessment Test
📚 Expert Articles
Read Our Blog
🎓 Learn at your pace